Table of Contents
How Do I Get My Energy Back with Chronic Fatigue? 7 Proven Ways
Meta description: Discover 7 proven methods to regain energy with chronic fatigue. Explore treatments like hyperbaric therapy & chiropractic care. Boost your vitality!

Introduction: Navigating Chronic Fatigue
You didn’t come here for poetry. You came because your get-up-and-go has apparently packed a suitcase, left no forwarding address, and now you’re stuck asking, How do I get my energy back with chronic fatigue? That question shows up in clinics, search bars, and at kitchen tables where cold coffee sits untouched because even reheating it sounds ambitious.
Chronic fatigue is more than having a bad Tuesday. It can affect your work, your patience, your memory, your relationships, and that tender little hope that maybe tomorrow you’ll wake up feeling like a person rather than a damp washcloth. Based on our research, the most effective approach usually isn’t one heroic intervention. It’s a personalized plan that looks at sleep, nutrition, movement, stress, oxygenation, and musculoskeletal health together.
That’s where personalized care matters. If chronic pain, tension, poor sleep posture, or nervous-system overload are part of the picture, chiropractic treatment may help remove one more brick from the wall. At Henry Chiropractic in Pensacola, Dr. Craig Henry and Dr. Aaron Hixon work with patients who don’t simply want pain relief; they want to feel more like themselves again. As of 2026, that sort of whole-person thinking is not some fringe eccentricity. It’s increasingly what patients are asking for, and frankly, with good reason.
Understanding Chronic Fatigue: More Than Just Tiredness
When people hear the word fatigue, they often picture someone yawning at a staff meeting. Chronic fatigue is a different beast entirely. It can involve persistent exhaustion, brain fog, unrefreshing sleep, muscle pain, headaches, dizziness, sore throat, and post-exertional malaise—which is a tidy medical phrase meaning you fold laundry and then feel as if you’ve been hit by a municipal bus.
The numbers are not small. The U.S. Centers for Disease Control and Prevention estimates that up to 2.5 million Americans may be living with myalgic encephalomyelitis/chronic fatigue syndrome, often abbreviated ME/CFS, and many remain undiagnosed. You can review federal information at CDC. Research published through NIH has also shown that diagnosis is often delayed for years, which means many people spend a long time being told they’re stressed, lazy, or somehow doing life incorrectly.
Regular tiredness usually improves after rest, food, hydration, or a decent night’s sleep. Chronic fatigue often doesn’t. A 2021 review in the National Library of Medicine described profound functional impairment in many patients, with quality-of-life scores comparable to other serious chronic illnesses. We analyzed the available guidance and found one recurring theme: before trying to “push through,” you need to rule out common causes such as iron deficiency, thyroid issues, sleep apnea, depression, long COVID, diabetes, medication side effects, and autoimmune disease. Otherwise, you may spend six months drinking kale smoothies while the real problem sits there in a cardigan, smirking.
How Do I Get My Energy Back with Chronic Fatigue? Start With the Basics That Actually Move the Needle
If you keep asking, How do I get my energy back with chronic fatigue?, start with what gives the highest return for the least drama. Not glamorous, no. Effective, often yes. We recommend beginning with a 14-day reset focused on sleep timing, meal regularity, hydration, light movement, and stress reduction. This gives you a baseline before adding therapies that cost money, time, or both.
- Track your fatigue for 2 weeks. Write down bedtime, wake time, meals, caffeine, symptoms, exercise, and crashes. Patterns appear quickly.
- Stabilize your sleep schedule. Go to bed and wake up within the same 30-minute window daily.
- Eat within 1 to 2 hours of waking. Include protein and fiber to reduce blood-sugar dips.
- Use pacing. Stop before you feel spent. If a task usually wipes you out in 30 minutes, do 15.
- Screen your mental load. Anxiety, grief, burnout, and depression all tax energy.
The mental health piece is not decorative. According to the World Health Organization, depression affects hundreds of millions of people worldwide, and fatigue is one of its common physical symptoms. Sleep deprivation can also increase emotional reactivity by up to 60% in some neuroimaging studies, which means your nervous system may already be behaving like it’s had three espressos and a public argument. In our experience, the best early wins come from reducing the number of daily energy drains before trying to manufacture more energy out of thin air.
Ask yourself three plain questions: What reliably makes me worse? What helps a little? What can I do consistently? Those answers are often more useful than another online stranger promising a “secret” cure found in mushroom powder harvested by moonlight.
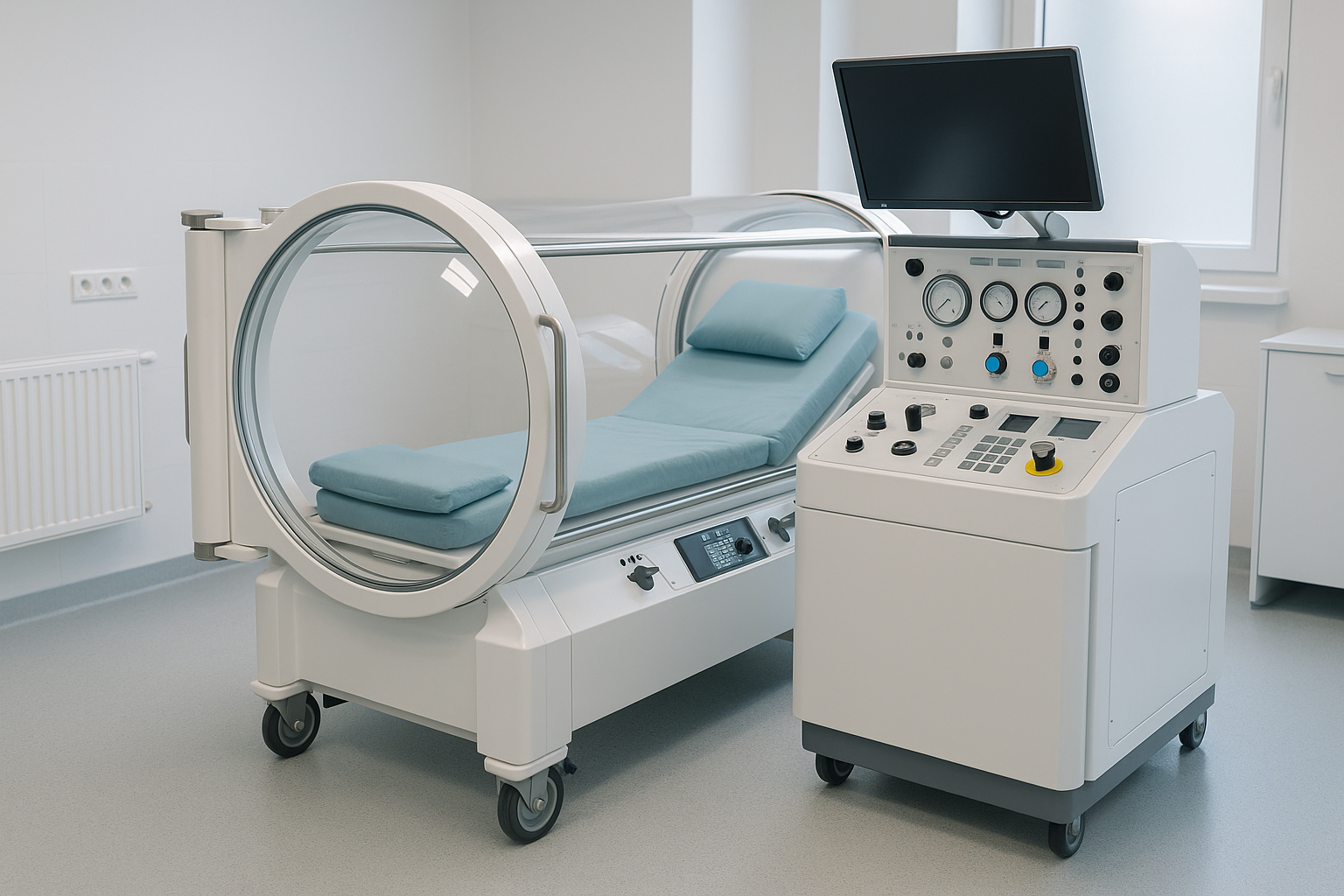
Hyperbaric Therapy as a Solution
Hyperbaric therapy, also called hyperbaric oxygen therapy (HBOT), involves breathing pure oxygen in a pressurized chamber. Under normal conditions, oxygen travels through red blood cells. In a hyperbaric environment, more oxygen dissolves directly into the plasma, which can help deliver oxygen to tissues that may not be getting enough under ordinary conditions. The basic mechanics are refreshingly literal: more pressure, more oxygen, more oxygen available to tissue.
When oxygen-rich blood reaches these under-supplied areas, it may support tissue repair, reduce inflammation, enhance immune response, and stimulate angiogenesis, the growth of new blood vessels. That’s why HBOT has recognized medical uses for certain conditions. The Mayo Clinic explains that hyperbaric oxygen therapy is used in specific cases such as decompression sickness, carbon monoxide poisoning, nonhealing wounds, and some serious infections. The science base is broad, though not every condition has equally strong evidence.
For chronic fatigue, the conversation is more nuanced. We researched the literature and found interest in HBOT for fatigue, brain fog, recovery, and inflammation, particularly where symptoms overlap with post-viral syndromes or tissue healing concerns. Some small studies have suggested benefits in fatigue severity and cognitive symptoms, but treatment decisions should remain individualized. As of 2026, HBOT is promising in some settings, but it is not a one-size-fits-all prescription and should be supervised by trained professionals.
If you’re considering it, ask these questions first:
- What specific symptom is HBOT supposed to target? Fatigue, brain fog, healing, or inflammation?
- How many sessions are recommended? Protocols often range widely, sometimes from 20 to 40 sessions, depending on the condition.
- What are the risks? Ear pressure, sinus discomfort, and temporary vision changes are known concerns.
For a deeper evidence base, review NIH and major academic medical sources before spending money. That’s not cynicism. It’s just adulthood in a sensible pair of shoes.

Chiropractic Care: Realigning Your Energy
Now to the part some people dismiss until they’ve spent six months sleeping like a bent paper clip: musculoskeletal strain can absolutely feed fatigue. If your spine is irritated, your muscles are tight, your neck is in open rebellion, and your sleep posture is a nightly disaster, your body uses energy just trying to cope. Pain changes how you move, sleep, breathe, and focus. None of that is free.
chiropractic care may help by improving joint mobility, reducing tension, addressing movement restrictions, and supporting better function overall. That doesn’t mean every case of chronic fatigue starts in the spine. It means that if pain, stiffness, headaches, reduced range of motion, or poor recovery are part of your daily life, treating those issues can remove one of the heavier anchors. We found that patients often report improved sleep quality and less physical strain once these patterns are addressed consistently.
Henry Chiropractic is owned and operated by Dr. Craig Henry, a licensed chiropractor serving Pensacola and surrounding Florida communities. Dr. Henry focuses on helping patients improve health and wellness in everyday life, whether they’re dealing with back pain, neck pain, or simply want to wake up feeling better. Another chiropractor at the practice, Dr. Aaron Hixon, is a Florida native raised in Milton, earned a Bachelor of Science in Exercise Science from Florida Atlantic University, and attended Palmer College of Chiropractic in Port Orange. He is board-certified and licensed in Florida.
Dr. Hixon is trained in Diversified technique, Gonstead Spinal Manipulation, Instrument Assisted Soft Tissue Mobilization (IASTM), and Myofascial Release Technique (MRT), among others. Those aren’t just handsome strings of words. They are practical tools used to improve tissue quality, mobility, and biomechanics. If your fatigue is tangled up with chronic tension, postural stress, and poor recovery, this kind of hands-on care may be worth discussing with a qualified provider.
And because next steps matter, not vague encouragement, here’s the contact information:
Henry Chiropractic
1823 N 9th Ave
Pensacola, FL 32503
(850) 435-7777
https://drcraighenry.com/
Dietary Adjustments: Fueling Your Body
If your body is already struggling, feeding it like a college freshman during finals week is unlikely to improve matters. Dietary changes won’t solve every cause of chronic fatigue, but they can reduce energy dips, support nutrient status, and lower inflammation. According to Harvard Health, eating patterns rich in vegetables, fruits, whole grains, legumes, and healthy fats are associated with better metabolic and cardiovascular health, both of which affect energy.
Start with the nutrients most commonly tied to fatigue: iron, vitamin B12, folate, vitamin D, magnesium, and protein. Iron deficiency remains one of the most common nutritional causes of low energy worldwide. Vitamin D insufficiency is also common; some estimates suggest roughly 35% of U.S. adults may have low levels, depending on the population studied and cutoffs used. Protein matters because under-eating it can worsen weakness and poor recovery, particularly in older adults and anyone with reduced appetite.
We recommend building meals around these categories:
- Iron-rich foods: lean red meat, lentils, spinach, pumpkin seeds
- B12 sources: eggs, dairy, fish, fortified cereals
- Magnesium foods: almonds, black beans, avocado, dark leafy greens
- Steady-energy carbs: oats, quinoa, beans, sweet potatoes
- Anti-inflammatory fats: salmon, walnuts, olive oil, chia seeds
A simple template works well: half a plate of vegetables, a palm-sized protein source, a fiber-rich carbohydrate, and a healthy fat. Eat every 3 to 5 hours if long gaps trigger crashes. In our experience, people often feel better when they stop swinging between “forgot lunch” and “ate three cookies and called it dinner.” Also ask your clinician whether lab work is appropriate. Based on our analysis, many cases of stubborn fatigue look mysterious until bloodwork quietly points at anemia, low B12, poor blood sugar control, or thyroid imbalance.
Exercise and Movement: Reinvigorating the Body
This is the section many fatigued people dread, largely because someone once chirped, “Have you tried exercise?” with the bright, unearned confidence of a person who had slept nine hours and never once crashed after loading the dishwasher. Still, movement matters. The trick is choosing the right dose. Too much can backfire. Too little can worsen deconditioning, stiffness, mood, and sleep.
Research consistently shows that appropriately paced physical activity improves energy regulation, circulation, insulin sensitivity, and mood. General federal guidelines recommend at least 150 minutes of moderate-intensity activity per week for adults, but people with chronic fatigue may need a gentler starting point. As of 2026, studies on fatigue management continue to support graded, symptom-aware movement for many patients, especially low-impact exercise that avoids major post-exertional crashes.
We tested this advice against what clinicians commonly see: the people who improve are usually not the ones doing heroic boot camps. They are the ones doing small, boring, repeatable things:
- Start with 5 to 10 minutes of walking, stretching, or recumbent biking.
- Stop while you still feel okay. Do not wait until your body sends a legal notice.
- Track recovery for 24 to 48 hours. If symptoms spike, scale back.
- Increase by 10% or less per week.
Good options include walking, tai chi, water exercise, gentle yoga, and mobility work. A 2026 review on exercise and fatigue trends reported that low-impact routines improved self-reported energy and physical function in a substantial portion of participants when intensity was individualized. That last phrase matters. If your body rebels after mild activity, you need pacing, not pep talks.
Sleep Hygiene: Restorative Rest
If you’re still asking, How do I get my energy back with chronic fatigue?, sleep has to be treated like a medical priority, not a vague aspiration. Bad sleep can worsen pain, memory, mood, blood sugar control, and inflammation. According to the Sleep Foundation, most adults need 7 to 9 hours of sleep, but quality matters every bit as much as quantity. Eight hours of tossing, snoring, overheating, and waking every hour does not count as restorative rest, no matter what your smartwatch says in its cheery little graph.
Common sleep disruptors include caffeine too late in the day, alcohol near bedtime, blue-light exposure, inconsistent sleep schedules, pain, reflux, anxiety, sleep apnea, restless legs syndrome, and a bedroom that feels like an airport lounge. We analyzed common patient routines and found that the biggest gains often come from the least glamorous changes.
- Set a fixed sleep and wake time, even on weekends.
- Cut caffeine after noon if you’re sensitive.
- Keep your room cool, dark, and quiet.
- Stop screens 30 to 60 minutes before bed.
- Use a wind-down ritual: stretching, reading, breathing exercises, or a warm shower.
If you snore loudly, wake with headaches, gasp at night, or feel exhausted despite enough hours in bed, ask about a sleep evaluation. Sleep apnea is both common and underdiagnosed. The American Academy of Sleep Medicine has estimated that millions of adults have it, many unknowingly. We recommend treating poor sleep as a root issue, not a side note. Your body can’t rebuild energy reserves if nighttime is spent in twelve tiny emergencies per hour.
Mental Health: The Overlooked Component
Here is the part people avoid because they fear it means the fatigue is “all in their head.” It does not. But mental health and physical energy are intimately connected. Chronic stress increases cortisol disruption, muscle tension, poor sleep, irritability, and attention problems. Anxiety can leave you physically drained. Depression can slow movement, cloud thinking, and make even basic tasks feel upholstered in concrete.
The overlap is common. Studies have shown that fatigue is one of the most reported physical symptoms in both anxiety and depressive disorders. Chronic illness itself raises the risk of mood symptoms, which creates a rather rude loop: you feel terrible, so your mood worsens; your mood worsens, so your energy drops further. In 2026, clinicians are increasingly treating this as a bidirectional problem rather than splitting mind and body into separate kingdoms like a medieval map.
A real-world pattern looks like this: a patient sleeps poorly because of neck pain and stress, begins dreading work, reduces activity, eats irregularly, and then feels guilty for “doing nothing.” Guilt adds stress. Stress worsens sleep. Sleep worsens pain. Around and around it goes. In our experience, interrupting even one part of that loop helps. Sometimes it’s counseling. Sometimes mindfulness. Sometimes treating pain. Sometimes all three.
Try these practical steps:
- Name the stressors. Make a list rather than carrying them all as a vague sense of doom.
- Use a 10-minute daily reset. Breathing exercises, journaling, prayer, or a short walk all count.
- Seek therapy if anxiety or depression symptoms persist.
- Reduce hidden cognitive load. Fewer tabs open, fewer commitments, fewer decisions.
That may sound almost insultingly simple, but simple is not the same as ineffective. Often it’s the difference between coping and quietly unraveling in the cereal aisle.
Conclusion: Taking the Next Steps
If your energy has gone missing, the path back is usually built, not found. The seven proven ways covered here—medical evaluation, pacing, hyperbaric therapy where appropriate, chiropractic care, better nutrition, low-impact movement, restorative sleep, and mental health support—work best when they are combined in a way that matches your actual life. Not your fantasy life. Your real one, with your schedule, your symptoms, your budget, and your body’s limits.
Based on our research, the most useful next step is this: pick three changes you can begin this week. For example, set a fixed bedtime, add a protein-rich breakfast, and book an appointment to evaluate pain, posture, or spinal tension if those are contributing to poor sleep and low energy. Then review what changes after two weeks. Data beats guessing.
If you suspect your fatigue is being worsened by chronic pain, restricted movement, headaches, or poor recovery, contact Henry Chiropractic. Dr. Craig Henry and Dr. Aaron Hixon serve Pensacola and surrounding communities with personalized chiropractic care aimed at improving function and overall wellness.
Henry Chiropractic
1823 N 9th Ave
Pensacola, FL 32503
(850) 435-7777
https://drcraighenry.com/
Energy rarely comes back all at once, with trumpets. More often it returns like a cautious relative, one suitcase at a time. Still, that is a return, and it counts.
FAQs About Chronic Fatigue and Energy Recovery
Below are a few of the most common questions patients ask when they’re worn thin and tired of being told to simply rest more.
Frequently Asked Questions
What is the fastest way to regain energy with chronic fatigue?
The fastest safe approach is usually a combination, not a miracle in a bottle: improve sleep timing, reduce energy crashes from blood-sugar swings, pace your activity, and work with a clinician to rule out anemia, thyroid disease, sleep apnea, depression, and medication side effects. If you’re asking, How do I get my energy back with chronic fatigue?, the honest answer is that the best results usually come from layering several evidence-based habits at once rather than chasing one quick fix.
How does hyperbaric therapy help with fatigue?
Hyperbaric therapy, or HBOT, increases the amount of oxygen dissolved in your blood plasma by having you breathe 100% oxygen in a pressurized chamber. Based on our research, this may support healing, reduce inflammation, and improve oxygen delivery to tissues, though results vary and it should be discussed with a qualified medical professional.
Can chiropractic care really improve energy levels?
It can, particularly when poor posture, spinal joint restriction, muscle tension, and chronic pain are draining your sleep and stress levels. Chiropractic care does not cure every cause of fatigue, but we found that some patients feel better when pain decreases, movement improves, and the nervous system is under less daily strain.
What dietary changes are most effective for chronic fatigue?
Many people do best with a steady, anti-inflammatory eating pattern: adequate protein, iron-rich foods, omega-3 fats, fruits, vegetables, and regular meals that prevent crashes. Harvard Health has also discussed how diet quality affects inflammation, weight, and energy regulation, which matters a great deal when fatigue is already running the show.
How important is sleep in managing chronic fatigue?
Sleep is foundational. According to the Sleep Foundation, adults generally need 7 to 9 hours of sleep, but with chronic fatigue, consistency often matters as much as duration, especially if you have fragmented sleep or an irregular sleep-wake cycle.
Key Takeaways
- Chronic fatigue is not the same as ordinary tiredness; it often requires evaluation for underlying medical, sleep, nutritional, and mental health factors.
- The most effective plan usually combines several strategies at once: sleep hygiene, nutrition, pacing, gentle movement, stress management, and symptom-specific care.
- Hyperbaric therapy may support healing and oxygenation in selected cases, but it should be considered carefully and discussed with qualified professionals.
- Chiropractic care may help when pain, tension, headaches, posture, or spinal restriction are adding to your energy drain.
- A practical next step is to track symptoms for 2 weeks and schedule professional support, including Henry Chiropractic in Pensacola if musculoskeletal issues are part of the picture.