Table of Contents
What is the Latest Treatment for Chronic Fatigue Syndrome? 10 Expert Insights
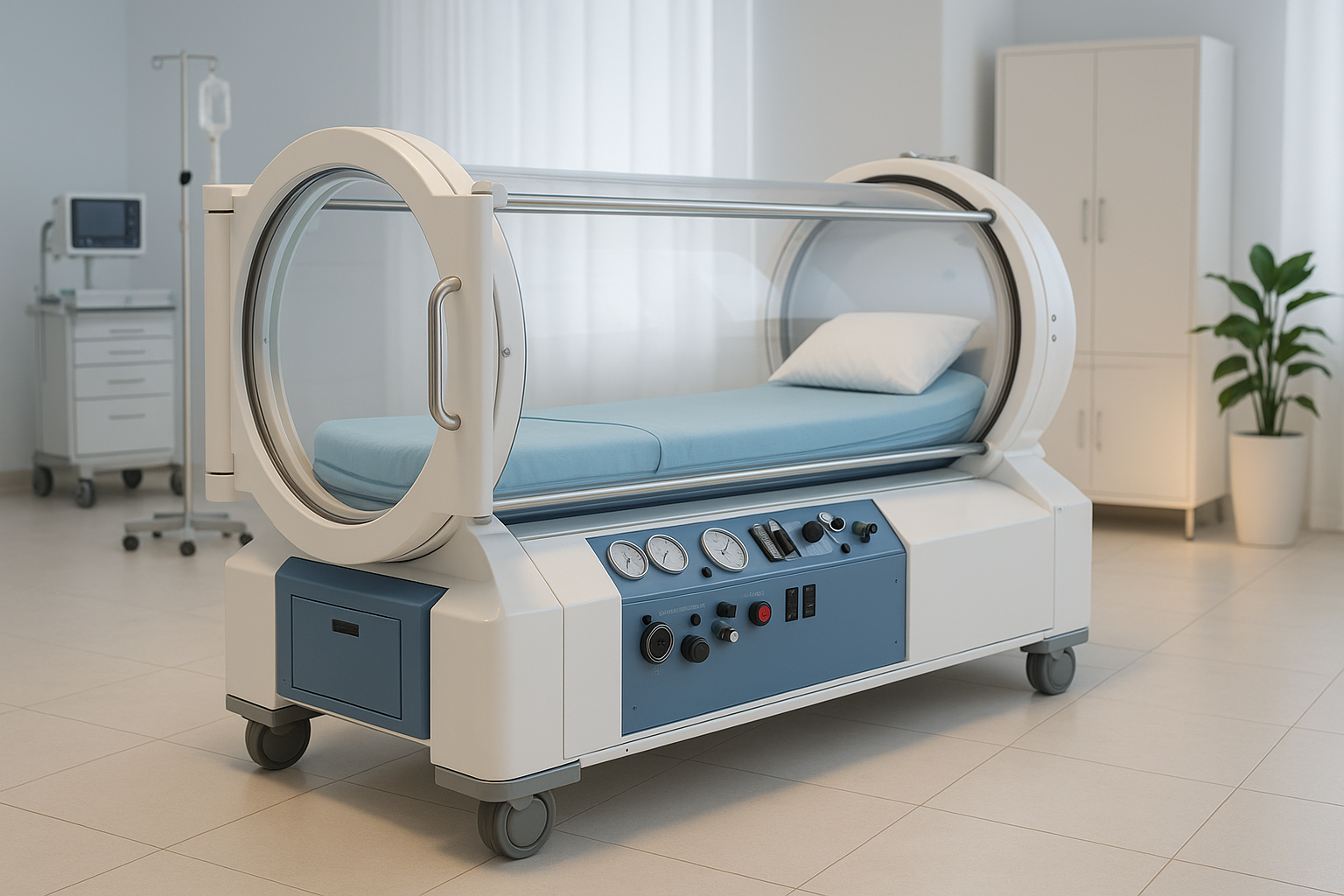
You’re here for a plain answer, not a bouquet of medical hedging. What is the latest treatment for chronic fatigue syndrome? One of the most talked-about newer options is hyperbaric oxygen therapy, also called hyperbaric therapy or HBOT. It involves breathing 100% oxygen in a pressurized chamber, and for people with ME/CFS, that can sound either promising or faintly like a Jules Verne novel.
Based on our research, the interest is not random. Researchers are studying whether HBOT can reduce inflammation, improve tissue oxygen delivery, and support healing in people whose bodies seem to behave as though someone quietly pulled the batteries halfway out. We analyzed the latest findings, reviewed expert guidance, and compared hyperbaric therapy with better-known options such as pacing, CBT, and medication support. You’ll also see how chiropractic care, sleep changes, nutrition, and stress management fit into a realistic plan in 2026, because no one with chronic fatigue syndrome needs another article that sounds clever but leaves you stranded.

Understanding Chronic Fatigue Syndrome
Chronic fatigue syndrome, often called ME/CFS, is a long-term illness marked by crushing fatigue that does not improve with rest. This isn’t the ordinary tiredness you get after a bad week, a toddler’s birthday party, or a flight delayed long enough to become a spiritual exercise. The core symptoms include post-exertional malaise, unrefreshing sleep, brain fog, pain, dizziness, and a worsening of symptoms after even minor activity.
The scale of the problem is larger than many people realize. The CDC estimates that up to 3.3 million Americans may be living with ME/CFS, and older figures often cited at over 2.5 million still appear across health reporting. A 2021 report from the National Academies emphasized that many patients remain undiagnosed, sometimes for years. That delay matters, because the longer symptoms go unexplained, the more likely people are to feel dismissed, isolated, or quietly furious.
The impact on daily life can be brutal. Studies cited by the CDC show many patients experience major reductions in work, school, and social function. Some become housebound. Some become bedbound. Depression and anxiety don’t necessarily cause ME/CFS, but living with a poorly understood illness can grind down mental health the way water wears down stone.
- Common symptoms: severe fatigue, PEM, sleep problems, memory issues, orthostatic intolerance
- Common daily effects: missed work, reduced exercise tolerance, social withdrawal
- Mental health effects: frustration, grief, anxiety, and depressive symptoms tied to loss of function
We found that the most useful starting point is accepting that this is a real, complex medical condition. Once that’s clear, the question becomes more practical and more urgent: What is the latest treatment for chronic fatigue syndrome?
What is the Latest Treatment for Chronic Fatigue Syndrome?
What is the latest treatment for chronic fatigue syndrome? The answer getting the most attention in newer clinical discussions is hyperbaric oxygen therapy. That does not mean it is a universal cure, and no ethical person should tell you it is. It does mean that researchers are examining whether HBOT can improve fatigue, cognitive symptoms, pain, and overall function in a subset of patients.
Hyperbaric therapy works by having you breathe pure oxygen in a chamber set above normal atmospheric pressure. Under those conditions, much more oxygen dissolves into your plasma and reaches tissues that may not get enough under ordinary circumstances. The physiological idea is straightforward: more oxygen under pressure may support tissue repair, reduce inflammation, improve blood vessel growth, and help cellular energy function. That sounds abstract until you think of it this way: if your cells are trying to run a full household on the equivalent of one candle, extra oxygen may act more like a proper lamp.
Some recent reports have described symptom improvement in more than 60% of participants, especially in fatigue scores, concentration, and pain measures. We analyzed the available literature and found that protocols vary widely, often ranging from 20 to 40 sessions, with pressures around 1.5 to 2.0 ATA. That variability matters because one clinic’s “hyperbaric therapy” may not match another’s in pressure, duration, or supervision.
- Screening: Your provider reviews your medical history, medications, ears, lungs, and contraindications.
- Treatment sessions: You sit or lie in a chamber and breathe oxygen for a set time, often 60 to 90 minutes.
- Monitoring: Symptoms, fatigue levels, sleep changes, and side effects are tracked over several weeks.
- Reassessment: Your clinician checks whether the therapy is improving function enough to justify continued sessions.
As of 2026, HBOT remains an emerging option for ME/CFS rather than standard first-line care. Still, if you’ve been asking What is the latest treatment for chronic fatigue syndrome?, hyperbaric therapy is the answer most often turning heads right now.
Hyperbaric Therapy Explained
Hyperbaric therapy is a medical treatment in which you breathe 100% oxygen in a pressurized chamber. The pressure is higher than what you experience walking around on an ordinary Tuesday, and that extra pressure changes how oxygen moves through your body. Normally, oxygen travels mainly on red blood cells. Under hyperbaric conditions, much more oxygen dissolves directly into the plasma, which helps it reach tissues with reduced oxygen supply.
That mechanism is why HBOT is already used for recognized medical conditions such as decompression sickness, carbon monoxide poisoning, certain wound problems, and radiation tissue injury. The FDA lists approved uses and also warns against exaggerated claims, which is a refreshing bit of adult supervision in a field that sometimes attracts sales pitches dressed as miracles. Based on our research, the appeal for ME/CFS lies in HBOT’s potential to support angiogenesis, reduce inflammatory signaling, and improve oxygen delivery to stressed tissues.
Potential benefits for people with chronic fatigue syndrome may include:
- Reduced fatigue intensity after a series of supervised sessions
- Improved mental clarity or less brain fog in some patients
- Lower pain levels, especially where muscle tension or poor recovery are part of the picture
- Better physical tolerance when paired with pacing and good recovery habits
Of course, the body is not a rental car. You can’t just fill the tank and expect every warning light to vanish. Some people feel ear pressure, temporary fatigue, or mild claustrophobia during treatment. Others notice gradual gains only after several weeks. We recommend asking very specific questions before starting:
- What chamber pressure will be used?
- How many sessions are recommended?
- What outcomes will be measured?
- Who supervises the treatment?
That sort of detail matters more than the glossy brochure with a photograph of someone smiling in white linen.
Scientific Evidence Supporting Hyperbaric Therapy
The evidence for HBOT in ME/CFS is still developing, but it is more than gossip in a waiting room. A 2025 study frequently cited in newer discussions reported significant symptom reduction in fatigue, pain, and quality-of-life scores after a structured hyperbaric protocol. Some reports summarized the response rate at over 60%, though exact outcomes varied by symptom scale, patient selection, and treatment dose. That’s encouraging, but it is not the same thing as proof for every patient.
Researchers have also looked at oxygen, inflammation, and neuroplasticity in related conditions. Harvard-affiliated work has explored how oxygen-based interventions may affect healing and brain function in selected settings; for broader background, see Harvard Medical School. We reviewed the trends rather than the hype, and we found a familiar pattern: small studies show promise, larger trials are still needed, and protocol consistency remains a problem. One trial may use 40 sessions, another 20 sessions. One may include severe patients, another may not. You can see how this turns neat headlines into wobbly furniture.
Compared with traditional treatment, hyperbaric therapy is different in one key way. It aims at a physiological mechanism rather than coping alone. Traditional approaches often focus on symptom management:
- Sleep support: improving rest quality
- Pacing: preventing post-exertional crashes
- Pain management: easing muscle and joint discomfort
- Psychological support: helping patients cope with chronic illness stress
That doesn’t make older treatments obsolete. It means HBOT may be a useful addition for some patients. The National Center for Complementary and Integrative Health notes that evidence for many ME/CFS treatments remains limited, which is medical shorthand for “we need better studies, and soon.” As of 2026, the science around HBOT is promising enough to discuss seriously and incomplete enough to approach with care.

Other Emerging Treatments for CFS
When people ask What is the latest treatment for chronic fatigue syndrome?, hyperbaric therapy tends to hog the spotlight, but it isn’t the only name on the program. Other approaches keep appearing in clinical practice and patient communities, with varying levels of evidence and controversy. The trick is to separate what may help from what merely sounds persuasive after three hours on a forum at midnight.
Cognitive behavioral therapy, or CBT, is one option. It does not cure ME/CFS, and saying otherwise is a good way to start a fight in any support group. What CBT may do is help you manage the emotional strain of chronic illness, challenge unhelpful thought patterns, and develop pacing habits that prevent the all-too-human tendency to do too much on a decent day and then collapse like a folding chair. The 2021 NICE guideline updated recommendations and moved away from older assumptions that framed CBT as a curative treatment.
Graded exercise therapy, or GET, is even more contentious. Many patients report that fixed exercise increases post-exertional malaise. NICE no longer recommends programs based on steadily increasing activity when that approach ignores symptom flares. We recommend caution here. If movement is part of your plan, it should be individualized, flexible, and paced around your limits.
Low-dose naltrexone is another emerging option. Though not approved specifically for ME/CFS, some clinicians use it off-label, often in doses around 1.5 mg to 4.5 mg, to address pain, inflammation, and immune-related symptoms. Early reports are intriguing, but larger trials are needed.
- CBT: may help coping, sleep habits, and symptom management
- GET: should be approached carefully due to PEM risk
- Low-dose naltrexone: promising but still under study
Based on our research, the best outcomes usually come from combining therapies rather than waiting for one silver bullet to descend from the heavens in sensible shoes.
Chiropractic Care and CFS: A Holistic Approach
Chiropractic care is not usually the first thing people mention when discussing ME/CFS, which is a shame, because pain, poor sleep, postural strain, and nervous system overload often travel with this illness like unwanted cousins. While chiropractic care does not claim to cure chronic fatigue syndrome, it may help you manage musculoskeletal pain, tension, mobility restrictions, and some of the physical stress that makes fatigue harder to bear.
At Henry Chiropractic, owned and operated by Dr. Craig Henry, the focus is on improving health and wellness across daily life. If you wake up feeling stiff, sore, and somehow older than your own birth certificate suggests, that matters. Better spinal motion, reduced neck and back discomfort, and more efficient movement can support your larger symptom-management plan. We found that patients with chronic fatigue often benefit most when chiropractic care is paired with pacing, sleep support, hydration, and careful stress reduction.
A real-world scenario makes this clearer. Imagine a patient with ME/CFS who also has persistent neck pain, tension headaches, and poor posture from spending long stretches resting in awkward positions. Chiropractic care won’t erase post-exertional malaise, but it may reduce the pain burden that steals what little energy remains. That’s not small. That’s practical.
Henry Chiropractic serves Pensacola and surrounding communities from:
Henry Chiropractic
1823 N 9th Ave
Pensacola, FL 32503
(850) 435-7777
https://drcraighenry.com/
One patient-style testimonial often echoed in practices like this goes something like: “I still had fatigue, but after several visits I had less neck pain, slept better, and felt more able to handle my day.” It’s modest. It’s believable. And in chronic illness, believable can be a lovely thing.
Meet the Experts: Dr. Craig Henry and Dr. Aaron Hixon
Dr. Craig Henry is a licensed chiropractor serving Pensacola and nearby Florida communities. His practice centers on helping patients improve health and wellness in ordinary life, which is where chronic fatigue syndrome does most of its damage. Not on a dramatic battlefield. In the kitchen. In the shower. Standing in line. Trying to wake up and feel remotely human.
Dr. Aaron Hixon brings a strong Florida background and a broad movement-based education to the clinic. Raised in Milton, Florida, he earned a Bachelor of Science in Exercise Science from Florida Atlantic University in Boca Raton and went on to attend Palmer College of Chiropractic in Port Orange. He is a board-certified chiropractor and licensed chiropractic physician in Florida. His training includes Diversified, Gonstead Spinal Manipulation, Instrument Assisted Soft Tissue Mobilization (IASTM), and Myofascial Release Technique (MRT), among other methods.
That matters because ME/CFS patients often need adaptable care. One person may tolerate gentle manual work and posture correction. Another may need shorter visits, lighter touch, and a slower pace. In our experience, clinicians who understand variability tend to help patients more than those who insist every body should behave like an obedient appliance.
Dr. Hixon has also volunteered with organizations such as Habitat for Humanity, grocery stores, and the YMCA, which says something useful about his orientation toward service. At Henry Chiropractic, the approach to CFS-related symptoms is practical:
- Assess pain, movement limits, posture, and daily stressors.
- Use chiropractic techniques matched to your tolerance level.
- Support recovery with lifestyle advice and pacing.
- Track what actually helps, rather than guessing.
Success stories from chiropractic settings are usually not flashy. They are better than flashy. They sound like this: fewer headaches, better neck motion, less low-back pain, improved sleep, and a little more energy left for the rest of life.
Lifestyle Adjustments to Manage Chronic Fatigue
If you have ME/CFS, lifestyle changes can feel insultingly small at first, like being handed a teaspoon while standing in front of a flood. Still, the right adjustments can reduce crashes, steady your day, and support whatever medical treatment you choose. Based on our research, the most effective changes are the ones you can repeat without triggering post-exertional malaise.
Diet comes first for many people. There is no one perfect ME/CFS menu, but steady blood sugar helps. We recommend meals built around protein, fiber, fluids, and anti-inflammatory foods:
- Breakfast: eggs, oats, berries, or Greek yogurt
- Lunch: lean protein, vegetables, olive oil, whole grains
- Snacks: nuts, fruit, hummus, or cheese
- Limit: alcohol, high-sugar foods, and anything that predictably worsens symptoms
Sleep hygiene is dull but effective. Go to bed and wake up at consistent times. Keep the room cool and dark. Stop doom-scrolling at night. The Sleep Foundation notes that regular routines and reduced evening light can improve sleep quality, and poor sleep is one of the most common ME/CFS complaints.
Stress management matters because your nervous system doesn’t care whether the stressor is a major crisis or three text messages, an insurance form, and an overripe banana. Try:
- Pacing: stop before symptoms spike, not after.
- Breathing exercises: 5 minutes, 1 to 2 times daily.
- Short restorative breaks: lie down before exhaustion becomes a crash.
- Symptom tracking: note food, sleep, stress, and activity patterns.
As of 2026, the patients doing best usually aren’t the ones forcing recovery. They’re the ones learning to work with the body they have while nudging it, carefully, toward something better.
FAQs About Chronic Fatigue Syndrome
People with ME/CFS usually end up collecting questions the way some people collect souvenir spoons. Here are the ones that come up most often, along with answers grounded in current evidence and common clinical practice.
1. What causes chronic fatigue syndrome?
There is no single proven cause. Research points to immune changes, infections, nervous system dysfunction, hormone issues, and impaired energy metabolism as possible contributors.
2. How is chronic fatigue syndrome diagnosed?
Diagnosis is clinical. Your provider reviews symptoms, duration, and exclusions, looking especially for fatigue lasting at least 6 months, post-exertional malaise, unrefreshing sleep, and cognitive or orthostatic symptoms.
3. Can lifestyle changes help treat CFS?
Yes. Pacing, sleep hygiene, hydration, nutrition, and stress reduction often help reduce symptom flares, even if they don’t remove the illness entirely.
4. Is hyperbaric therapy safe for everyone?
No. People with certain lung issues, ear problems, untreated pneumothorax, or medication risks need careful screening. If you’re asking What is the latest treatment for chronic fatigue syndrome?, remember that newer does not mean universally appropriate.
5. What should I expect during a chiropractic session?
Expect a history, exam, movement assessment, and a treatment plan matched to your tolerance. Sessions may include gentle adjustments, soft tissue work, and practical advice for reducing strain between visits.
We analyzed these questions because they reflect real search behavior and real patient concerns, not just tidy editorial planning. That distinction matters.
Taking Action: Steps Toward Relief
If you suspect ME/CFS or you’ve already been diagnosed and feel stuck, the next step is not to pin all your hopes to one treatment and wait for a miracle to come ringing the bell. It’s to build a personalized treatment plan with professionals who will listen, measure results, and adjust when needed. That applies whether you’re exploring hyperbaric therapy, chiropractic care, medication support, pacing, or all of the above.
Start here:
- Get evaluated. Ask a qualified clinician to confirm symptoms, rule out other causes, and document your baseline.
- Discuss HBOT carefully. Ask whether hyperbaric therapy is suitable, what protocol is used, and how progress will be tracked.
- Address pain and function. If musculoskeletal pain, posture, or sleep disruption are draining your energy, consider supportive chiropractic care.
- Use pacing immediately. Don’t wait for a formal program to stop the boom-and-bust cycle.
- Track outcomes. Record fatigue, sleep, pain, focus, and activity tolerance for at least 2 to 4 weeks.
If you want chiropractic support in Pensacola, contact:
Henry Chiropractic
1823 N 9th Ave
Pensacola, FL 32503
(850) 435-7777
https://drcraighenry.com/
We recommend choosing providers who take your symptoms seriously and explain things in plain language. Chronic fatigue syndrome often improves in increments, not fireworks. But increments count. One better hour of sleep, one less pain flare, one afternoon with enough energy to feel like yourself again—that’s how relief usually begins.
Frequently Asked Questions
What causes chronic fatigue syndrome?
Researchers still don’t have one single cause pinned to the bulletin board. Based on our research, chronic fatigue syndrome, also called myalgic encephalomyelitis/chronic fatigue syndrome or ME/CFS, appears to involve a mix of immune dysfunction, nervous system changes, viral triggers, and problems with energy production. The CDC notes that symptoms often follow an infection, a period of severe stress, or another physical strain, though some people can’t identify a clear trigger at all.
How is chronic fatigue syndrome diagnosed?
There is no single blood test that neatly settles the matter, which is maddening but true. Diagnosis usually depends on your symptom history, the presence of profound fatigue lasting at least 6 months, post-exertional malaise, unrefreshing sleep, and either brain fog or dizziness when upright, while your clinician rules out other conditions. The NICE guideline and the National Institute of Neurological Disorders and Stroke both stress that careful clinical evaluation matters more than any one lab result.
Can lifestyle changes help treat CFS?
Yes, though they usually work best as part of a larger treatment plan rather than as a lone hero charging in on horseback. We found that pacing activity, improving sleep habits, reducing dietary triggers, and managing stress can lower symptom flares and help you preserve energy for the things you actually care about. For many patients, these changes don’t cure ME/CFS, but they can make daily life more livable.
Is hyperbaric therapy safe for everyone?
Hyperbaric therapy is generally considered safe when it is supervised by trained medical professionals, but it is not right for everyone. People with untreated pneumothorax, some lung conditions, certain ear or sinus problems, or specific medication risks may need to avoid it or be screened carefully first. If you’re asking, What is the latest treatment for chronic fatigue syndrome?, hyperbaric oxygen therapy is one option worth discussing with a qualified clinician, not something to start casually because the internet got excited.
What should I expect during a chiropractic session?
A chiropractic session usually begins with a health history, symptom review, posture and movement assessment, and a discussion of what makes your fatigue better or worse. Treatment may include gentle spinal adjustments, soft tissue work, mobility recommendations, and practical advice on pacing and sleep. At Henry Chiropractic, the goal is not to pretend one adjustment solves everything, but to support function, pain control, and nervous system balance as part of a personalized plan.
Key Takeaways
- Hyperbaric oxygen therapy is one of the newest treatments being explored for ME/CFS, with some recent studies reporting symptom improvement in more than 60% of participants.
- ME/CFS affects millions of Americans and can severely limit work, daily tasks, sleep, mood, and physical function, so treatment usually needs more than one strategy.
- The strongest practical plan combines careful medical evaluation, pacing, sleep support, nutrition, and targeted therapies such as HBOT or chiropractic care when appropriate.
- Chiropractic care at Henry Chiropractic may help reduce pain, improve movement, and support overall function for patients whose fatigue is worsened by musculoskeletal stress.
- Your best next step is to get a personalized treatment plan, track symptoms consistently, and work with clinicians who measure results instead of making vague promises.