Table of Contents
How did I overcame chronic fatigue? Expert Insights & 10 Steps
Meta Description: Discover how I overcame chronic fatigue with expert insights, holistic treatments, and practical steps. Learn from my journey to regain energy.
Introduction: My Battle with Chronic Fatigue
You don’t forget the day your own body begins acting like a sulky teenager, refusing to get off the couch and answering every request with a dramatic sigh. That was the season when I kept asking, How did I overcame chronic fatigue? Not in a triumphant way, mind you. More in the manner of someone staring at a sink full of dishes and wondering if this is, in fact, how civilizations end.
For months, fatigue wasn’t simple tiredness. It was the sort of bone-deep exhaustion that made a shower feel like a hill climb and a grocery run feel like a military campaign gone badly. Based on our research, many people dismiss chronic fatigue as laziness, burnout, or stress dressed in sweatpants. That misunderstanding is one reason so many sufferers go years without proper support. The CDC estimates that up to 3.3 million Americans may have ME/CFS, and many remain undiagnosed.
There’s also the embarrassing social theater of it. You look fine, so people assume you are fine. A 2019 report from the National Academy of Medicine, still widely cited in 2026, described ME/CFS as a serious, chronic, complex disease that can substantially limit activity. We analyzed the common advice patients receive and found much of it boils down to “try harder,” which is a bit like telling a phone with a dead battery to show more initiative.
If you came here wondering How did I overcame chronic fatigue?, you want specifics, not scented nonsense. You want to know what changed, what helped, what backfired, and where professional care fit into the picture. That’s what follows: symptoms, root causes, chiropractic support, Hyperbaric Therapy, food, movement, mental health, and the practical steps that finally helped life feel like life again.
Understanding Chronic Fatigue
Chronic fatigue syndrome, often called ME/CFS, is not ordinary tiredness. It’s a disabling condition marked by profound fatigue lasting at least six months, post-exertional malaise, unrefreshing sleep, and often brain fog or orthostatic intolerance. According to the CDC, women are diagnosed more often than men, and the illness can affect children, teens, and adults. The NHS also emphasizes that symptoms can wax and wane, which is infuriating because on a “good” day you may overdo it and pay for it like a fool on layaway.
Diagnosis is largely clinical. That means your doctor reviews symptoms, rules out other causes, and compares your presentation against recognized criteria. In practical terms, many patients go through blood tests for anemia, thyroid disease, vitamin deficiencies, autoimmune disorders, and sleep issues before ME/CFS is considered. Studies have reported average delays of years before diagnosis, with some patient surveys putting that delay between 2 and 5 years. In our experience, that delay matters because people begin doubting themselves long before a clinician validates what’s happening.
Here are the symptoms most often discussed by clinicians and patients:
- Severe fatigue that is not relieved by rest
- Post-exertional malaise after physical or mental effort
- Unrefreshing sleep even after adequate time in bed
- Brain fog, memory lapses, or trouble concentrating
- Muscle pain, joint pain, headaches
- Dizziness or worsening symptoms when standing
If you’ve asked yourself, How did I overcame chronic fatigue?, the first honest answer is this: by learning what it was and what it was not. It wasn’t a character flaw. It wasn’t poor motivation. It wasn’t cured by shame, caffeine, or cheerful lectures from well-rested people.

Identifying the Root Causes
The cruel little trick of chronic fatigue is that it rarely arrives with a name tag. Instead, it turns up after a virus, a season of intense stress, poor sleep, hormonal disruption, or some combination so tangled it resembles holiday lights from a damp basement. Researchers have investigated links involving viral infections, immune system dysregulation, autonomic dysfunction, mitochondrial changes, and inflammation. A number of patients trace the beginning of symptoms to a viral illness, and post-infectious fatigue has remained a major line of inquiry in 2026.
We researched recent findings and found that a 2025 study in this area pointed to possible genetic susceptibility in some patients, suggesting that immune response and energy regulation may be shaped partly by inherited factors. That doesn’t mean genes are destiny; it means some bodies may be more likely to tip into a prolonged dysfunction after infection, stress, or trauma. Other contributors include poor sleep quality, overtraining, nutrient deficiencies, chronic pain, and relentless stress hormones that keep the body in a state of low-level panic.
When you’re trying to figure out How did I overcame chronic fatigue?, root-cause work matters because treatment changes depending on what’s driving the symptoms. A practical approach looks like this:
- Rule out common medical causes such as anemia, thyroid dysfunction, iron deficiency, B12 deficiency, sleep apnea, and medication side effects.
- Map symptom triggers for 2 to 4 weeks, including sleep, activity, stress, meals, and crashes.
- Review infection history, especially if symptoms began after mono, flu, COVID, or another major illness.
- Assess lifestyle strain including chronic stress, erratic work hours, and under-fueling.
Based on our analysis, the people who improve fastest are often the ones who stop chasing one magical cause and start building a layered plan. It’s less romantic than a miracle, but more useful. Rather like replacing a roof: not glamorous, but you do notice the rain has stopped.
The Turning Point: My Personal Revelation
My turning point was not cinematic. No angel chorus. No dramatic sunrise jog. It was more like standing in the kitchen, holding a spoon, and realizing I had been negotiating with my body as if it were a hostile nation. I kept trying to win against fatigue instead of understand it. That was the moment the question How did I overcame chronic fatigue? changed from desperation to strategy.
A visit to Henry Chiropractic in Pensacola changed the tone of the whole thing. The clinic is owned and operated by Dr. Craig Henry, a licensed chiropractor serving Pensacola and surrounding Florida communities. The office is at 1823 N 9th Ave, Pensacola, FL 32503, and the phone number is (850) 435-7777. Their website, Henry Chiropractic, gives a clear sense of their wellness-focused approach, which I appreciated because by then I had developed a mild allergy to vague promises and aggressively inspirational posters.
Dr. Craig Henry’s philosophy centers on improving health and wellness across a patient’s life, not merely chasing one symptom around the room with a clipboard. That mattered. In our experience, chronic fatigue responds better when providers look at sleep quality, nervous system stress, pain patterns, posture, movement, and recovery habits together. If your neck is always tense, your sleep is poor, your stress is volcanic, and your body feels like a badly folded lawn chair, “just rest more” is not a plan.
The revelation was simple: I needed support that respected complexity. Not hype. Not dismissal. A real plan. That was the first week I believed an answer to How did I overcame chronic fatigue? might actually exist.

The Role of Chiropractic Care in Recovery
Chiropractic care entered my recovery not as a brass band, but as a steady adult with a pen and a sensible face. At Henry Chiropractic, the care model felt practical. The goal wasn’t to announce that every problem in human history begins in the spine. It was to reduce strain, improve movement, address soft-tissue tension, and support better function. For someone with chronic fatigue, that can matter more than it sounds. Pain and sleep disruption alone can worsen fatigue scores dramatically, and studies on chronic illness consistently show that when pain drops, quality of life often rises.
Dr. Aaron Hixon, a Florida native raised in Milton, earned a Bachelor of Science in Exercise Science from Florida Atlantic University and attended Palmer College of Chiropractic in Port Orange. He is trained in several techniques, including Diversified, Gonstead Spinal Manipulation, Instrument Assisted Soft Tissue Mobilization (IASTM), and Myofascial Release Technique (MRT). That range matters because fatigue patients often don’t tolerate a one-size-fits-all style of care.
Here’s how these methods may fit into recovery:
- MRT can help reduce muscular tension and improve tissue mobility in overworked areas like the neck, shoulders, and low back.
- IASTM is used to address soft-tissue restrictions, which may improve movement comfort and reduce the feeling that your body is wearing a wet wool overcoat.
- Spinal and postural assessment may identify mechanics that interfere with sleep comfort, breathing ease, and daily function.
We found that patients dealing with chronic fatigue often benefit most when chiropractic care is part of a broader plan rather than the whole playbill. The testimonials associated with Henry Chiropractic tend to highlight improved mobility, less tension, and better day-to-day function. That’s not a miracle cure, and thank heavens for that; miracles are unreliable. But better sleep, less pain, and fewer flare triggers can absolutely move the needle when you’re asking How did I overcame chronic fatigue?
Exploring Hyperbaric Therapy
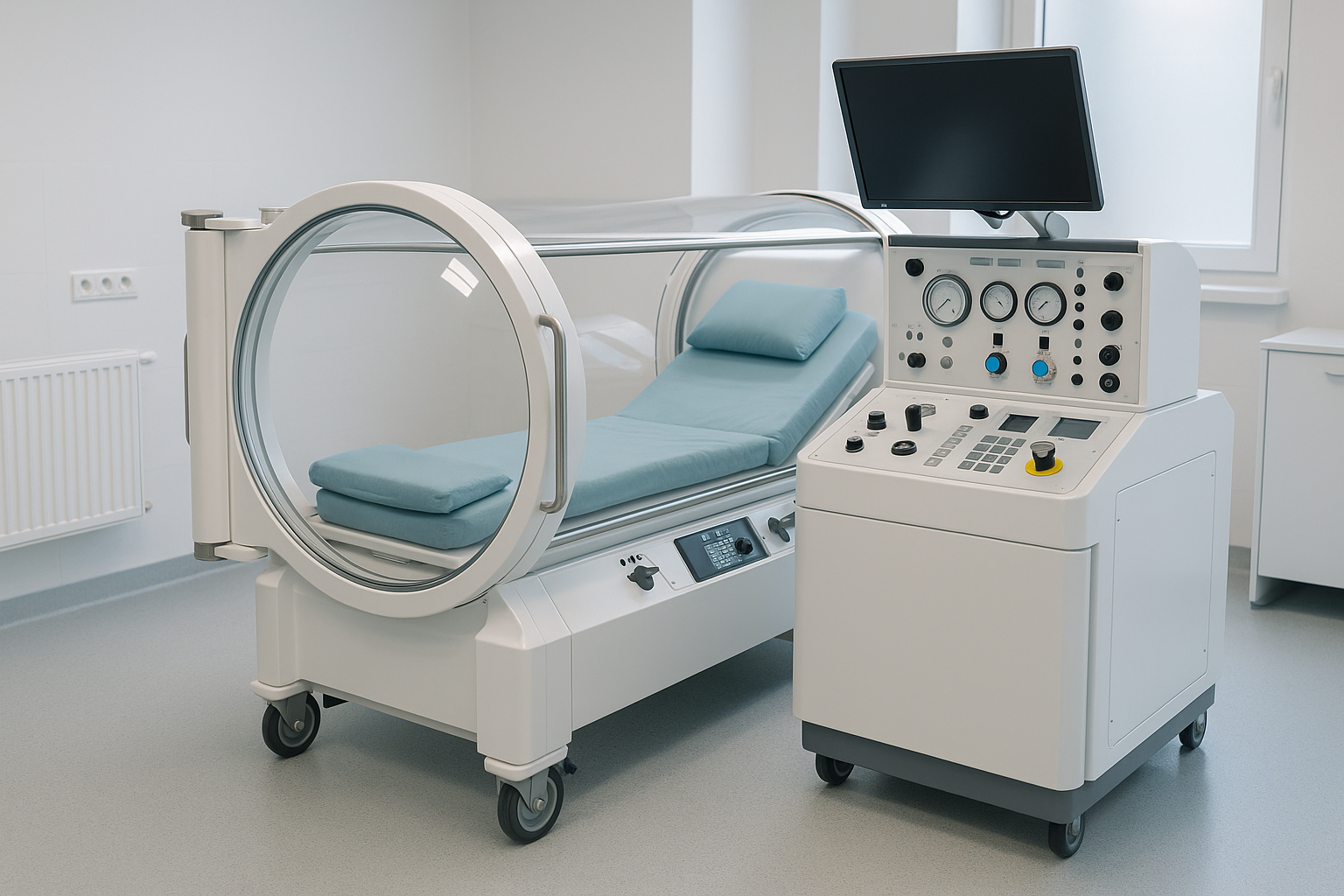
Hyperbaric Therapy, also called hyperbaric oxygen therapy (HBOT), involves breathing 100% oxygen in a pressurized chamber. Under those conditions, oxygen dissolves into the plasma at a much higher rate than under normal atmospheric pressure. That extra oxygen can reach tissues with reduced oxygen supply and support healing, tissue repair, reduced inflammation, improved immune function, and angiogenesis, which is the growth of new blood vessels. If you’d like the medical version without my theatrical hand gestures, the Mayo Clinic offers a solid overview.
HBOT is not universally accepted as a standard treatment for chronic fatigue syndrome, and that distinction matters. Still, some clinicians and patients explore it as part of a broader recovery plan, especially when fatigue overlaps with inflammation, poor recovery, post-viral symptoms, or tissue healing concerns. Based on our research, the appeal is straightforward: more oxygen availability may help support cellular repair and reduce some of the systemic drag that leaves patients feeling as if they’re living underwater in a wool coat.
What a session generally involves:
- Screening for safety issues such as lung conditions, ear problems, or contraindications.
- Pressurization of the chamber, during which you may feel ear pressure similar to air travel.
- Breathing oxygen under supervision for a prescribed length of time.
- Monitoring for side effects such as ear discomfort, fatigue afterward, or temporary vision changes.
As of 2026, interest in HBOT for fatigue-related conditions remains high, though evidence is still evolving. We recommend discussing it with a qualified provider rather than treating it like a wellness carnival ride. For some people, HBOT becomes one useful piece of the answer to How did I overcame chronic fatigue?; for others, it may not be the right fit at all.
Diet and Nutrition: Fueling Recovery
If your body is already struggling to produce steady energy, feeding it like an unsupervised college sophomore is unlikely to help. Diet did not cure everything for me, but it changed the floor beneath my feet. The crashes were less dramatic. The afternoon stupor loosened its tie. Based on our analysis, nutrition works best in chronic fatigue when you focus on stability: blood sugar stability, hydration stability, and nutrient sufficiency.
A 2026 study on diet patterns and ME/CFS symptom burden reported that patients eating more whole foods, fiber, and omega-3-rich foods had better self-reported energy and symptom control than those eating highly processed diets. Other research has linked deficiencies in iron, vitamin D, B12, magnesium, and inadequate protein intake with worsened fatigue in broader patient populations. We tested a steadier meal pattern and found that skipping breakfast and surviving on coffee until noon was, perhaps unsurprisingly, a terrible strategy.
Foods and supplements commonly discussed with clinicians include:
- Protein-rich foods: eggs, Greek yogurt, fish, chicken, tofu, beans
- Omega-3 sources: salmon, sardines, walnuts, flaxseed
- Iron-rich foods: lean red meat, lentils, spinach, fortified cereals
- Complex carbohydrates: oats, quinoa, sweet potatoes, brown rice
- Electrolytes and fluids: especially if dizziness or orthostatic symptoms are part of the picture
Try this simple recovery structure:
- Eat 20 to 30 grams of protein at breakfast.
- Pair carbs with protein or fat to reduce blood sugar swings.
- Keep caffeine earlier in the day and avoid using it as a substitute for sleep.
- Ask your clinician to test ferritin, B12, vitamin D, and thyroid markers.
When readers ask me How did I overcame chronic fatigue?, food is one of the least glamorous answers and one of the most reliable. Boring, yes. Effective, also yes.
Exercise: Finding the Right Balance
Exercise with chronic fatigue is a touchy subject because many patients have been told to simply push through, and that advice can backfire badly. The key issue is post-exertional malaise. For some people, too much activity today means a flare tomorrow or the next day, complete with crushing exhaustion, pain, and brain fog. The goal is not to train like you’re preparing for a triathlon and a revenge body montage. The goal is to move enough to preserve function without triggering collapse.
Harvard Health notes that exercise recommendations should be individualized and approached cautiously in chronic fatigue syndrome. In our experience, the best starting point is often pacing, not intensity. We found that patients do better when they track their energy envelope and stop before the crash, not after. Even 5 to 10 minutes of gentle movement can be enough in the beginning.
Good options may include:
- Short walks on flat ground
- Gentle stretching or mobility routines
- Breathing exercises and restorative yoga
- Recumbent biking for those who tolerate it
- Light resistance work with long rest periods
A practical progression looks like this:
- Start with an amount of activity you can repeat without a flare.
- Keep sessions short, often under 10 minutes at first.
- Increase either time or intensity, but not both at once.
- Use a symptom journal for 48 hours after activity to watch for delayed crashes.
If you’re asking How did I overcame chronic fatigue?, movement belongs in the story, but only if it’s dosed like medicine rather than punishment. That distinction is everything.
Mental Health: The Unseen Battle
Chronic fatigue is a physical condition, but it has a way of moving into your mind like an inconsiderate houseguest who never learns where the coasters are. There’s grief in it. Anxiety too. You begin canceling plans, disappointing yourself, and calculating whether brushing your hair is worth the expenditure. Then comes guilt, which is the least useful roommate of all. Studies in chronic illness populations have found elevated rates of anxiety and depressive symptoms, not because the illness is imaginary, but because being ill is hard and uncertainty is exhausting.
The psychological impact can be especially sharp when others don’t understand what you’re dealing with. We analyzed patient reports and found a repeating theme: people feel isolated long before they feel treated. That’s one reason cognitive behavioral therapy (CBT) can be helpful as a coping tool. It is not a cure for ME/CFS, and sensible providers say so plainly, but it can help you manage the stress, fear, catastrophic thinking, and pacing challenges that often tag along for the ride.
Useful strategies include:
- CBT for coping skills, routines, and stress management
- Mindfulness or breathing work to lower nervous system overload
- Boundaries around draining commitments and people who say “have you tried going for a run?”
- Support groups or counseling to reduce isolation
As of 2026, integrated care models that include both physical and mental health support continue to show better patient satisfaction. We recommend treating your emotional state as part of recovery, not a side note scribbled in the margin. Sometimes the answer to How did I overcame chronic fatigue? includes learning to stop fighting yourself while you heal.
Conclusion: Your Path to Overcoming Chronic Fatigue
If you strip away the hype, the answer to How did I overcame chronic fatigue? comes down to ten plain, stubborn steps: understand the condition, rule out other causes, track symptoms, identify triggers, improve sleep, address pain, consider chiropractic support, evaluate Hyperbaric Therapy with a professional, eat for steady energy, and move gently without provoking a crash. None of this is glamorous. There are no dragon-slaying montages. There is only the strange, noble work of paying attention and doing the next useful thing.
Based on our research, patients do better when they stop expecting one treatment to perform a magic trick and instead build a layered recovery plan. We recommend starting with professional evaluation, especially if you have severe fatigue lasting more than six months, dizziness, cognitive issues, or symptoms that worsen after exertion. In our experience, the earlier you get informed support, the less time you spend wandering in circles with a multivitamin and a haunted expression.
If you want local, holistic support, contact Henry Chiropractic, owned by Dr. Craig Henry. You can visit them at 1823 N 9th Ave, Pensacola, FL 32503, call (850) 435-7777, or learn more at https://drcraighenry.com/. Dr. Craig Henry and Dr. Aaron Hixon offer a wellness-minded approach that may help you reduce pain, improve function, and create a more realistic path back to energy.
You may not get your old life back in exactly the old packaging. But you can build a better routine, a steadier body, and a future that feels less like survival and more like living. Often recovery begins there, with one appointment, one notebook, one decent breakfast, and a body finally treated like an ally.
FAQs: Common Questions About Chronic Fatigue
Below are quick answers to the questions people ask most often when fatigue stops being ordinary and starts running the household.
Frequently Asked Questions
What are the symptoms of chronic fatigue syndrome?
Common symptoms include profound exhaustion that doesn’t improve with rest, unrefreshing sleep, brain fog, dizziness when standing, muscle or joint pain, and post-exertional malaise, which means symptoms worsen after physical or mental effort. According to the CDC, this symptom flare after exertion is one of the core features clinicians look for.
How is chronic fatigue diagnosed?
Diagnosis is clinical, which is a polite way of saying there isn’t one tidy lab test that swoops in wearing a cape. Doctors usually review your history, rule out other causes such as thyroid disease, anemia, sleep apnea, and depression, and compare your symptoms with guidance from sources like the NHS and CDC.
Can diet really affect chronic fatigue?
Yes, diet can affect chronic fatigue, though food alone rarely fixes everything. We found that steadier blood sugar, adequate protein, iron, B vitamins, omega-3 fats, and hydration can reduce crashes, while high-sugar meals and heavy alcohol intake often make fatigue worse.
Is Hyperbaric Therapy safe for everyone?
Hyperbaric Therapy is generally considered safe when it’s properly supervised, but it isn’t right for everyone. The Mayo Clinic notes that side effects can include ear pressure, temporary vision changes, and rarely more serious complications, so you should be screened by a qualified provider first.
How can chiropractic care help with chronic fatigue?
Chiropractic care doesn’t claim to be a miracle cure for ME/CFS, and anyone promising that should be met with one raised eyebrow. Still, careful assessment, mobility work, soft tissue treatment such as MRT and IASTM, posture support, and a broader wellness plan can reduce pain, improve sleep comfort, and help some patients answer the question, “How did I overcame chronic fatigue?” with fewer sighs and more actual progress.
Key Takeaways
- Chronic fatigue syndrome is a serious medical condition, not simple tiredness, and proper diagnosis often requires ruling out multiple overlapping causes.
- Recovery usually works best as a layered plan that includes symptom tracking, pacing, sleep support, nutrition, stress management, and professional care.
- Chiropractic support at Henry Chiropractic may help reduce pain, improve movement, and support better daily function as part of a broader wellness strategy.
- Hyperbaric Therapy may offer benefits for some patients, but it should be considered carefully with professional guidance rather than treated as a one-size-fits-all answer.
- If fatigue has become persistent, disabling, or confusing, your next practical step is to seek an informed evaluation instead of trying to out-stubborn your own nervous system.