Table of Contents
What Medical Conditions are Treated by Oxygen Therapy? The Expert Guide: 11 Essential Uses in 2026
You’re probably here because someone you love is short of breath, sleep deprived, slow to heal, or newly curious about a treatment that sounds faintly futuristic and yet has been around long enough to have acquired rules, studies, billing codes, and people who speak about it with a tone usually reserved for tax law. What medical conditions are treated by oxygen therapy? Quite a few, actually: COPD, severe asthma attacks, sleep apnea with low nighttime oxygen, diabetic wounds, certain brain injuries, and more.
In 2026, oxygen therapy matters even more because chronic lung disease, diabetes, and post-viral recovery remain stubbornly common. According to the CDC, millions of Americans live with COPD, and diabetes continues to drive a large burden of chronic wounds. Based on our research, patients aren’t just asking whether oxygen works; they want to know when it works, for whom it works, and whether hyperbaric therapy belongs in the same conversation.
Locally, Henry Chiropractic in Pensacola is part of that conversation. Dr. Craig Henry, who owns and operates the practice, and Dr. Aaron Hixon, a Florida-licensed chiropractic physician with a background in exercise science and hands-on rehabilitation methods, are known to local patients seeking conservative care and guidance on therapies that support recovery. If you want a sensible, medically grounded next step rather than internet folklore in a lab coat, they’re worth knowing.
Understanding Oxygen Therapy: The Basics
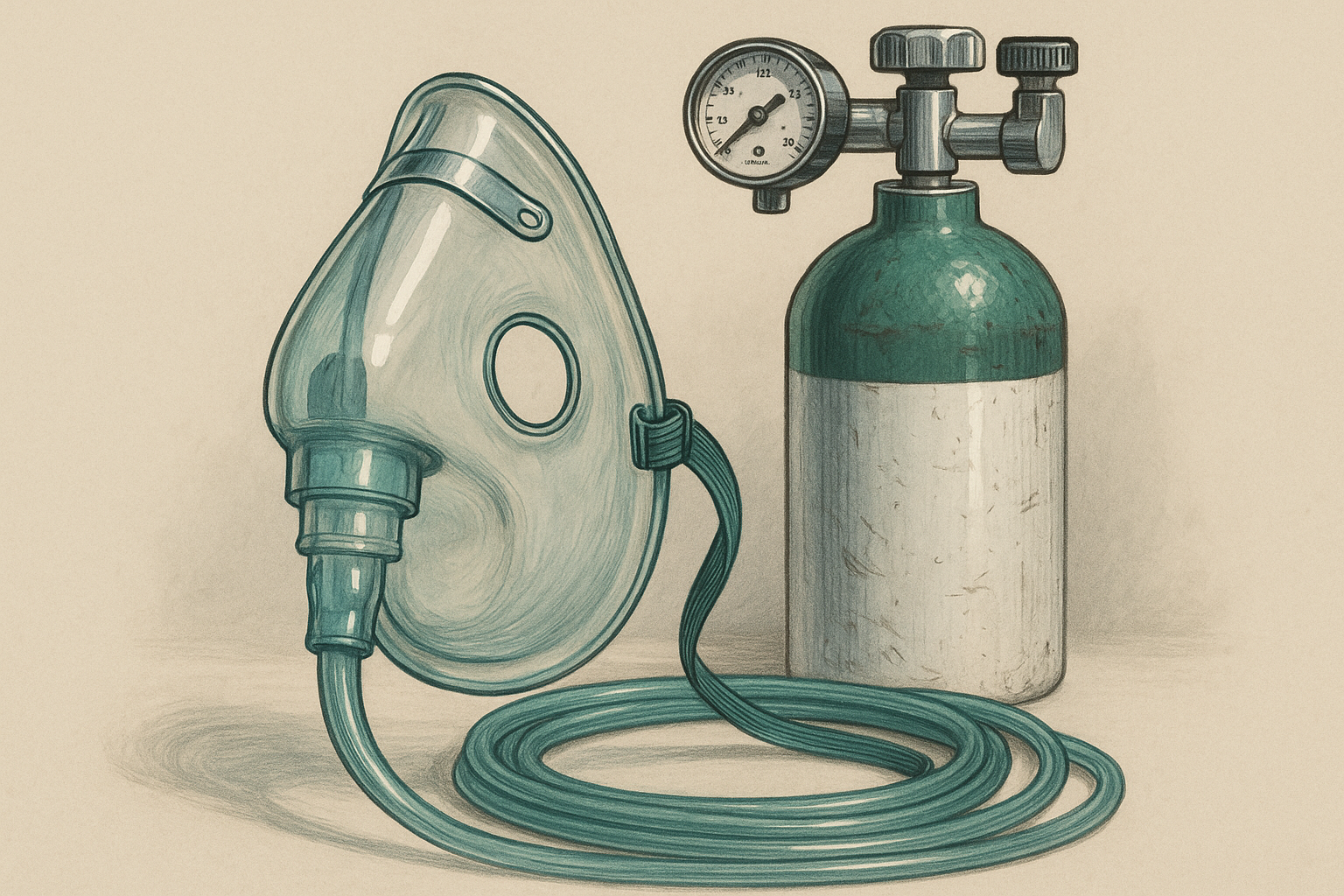
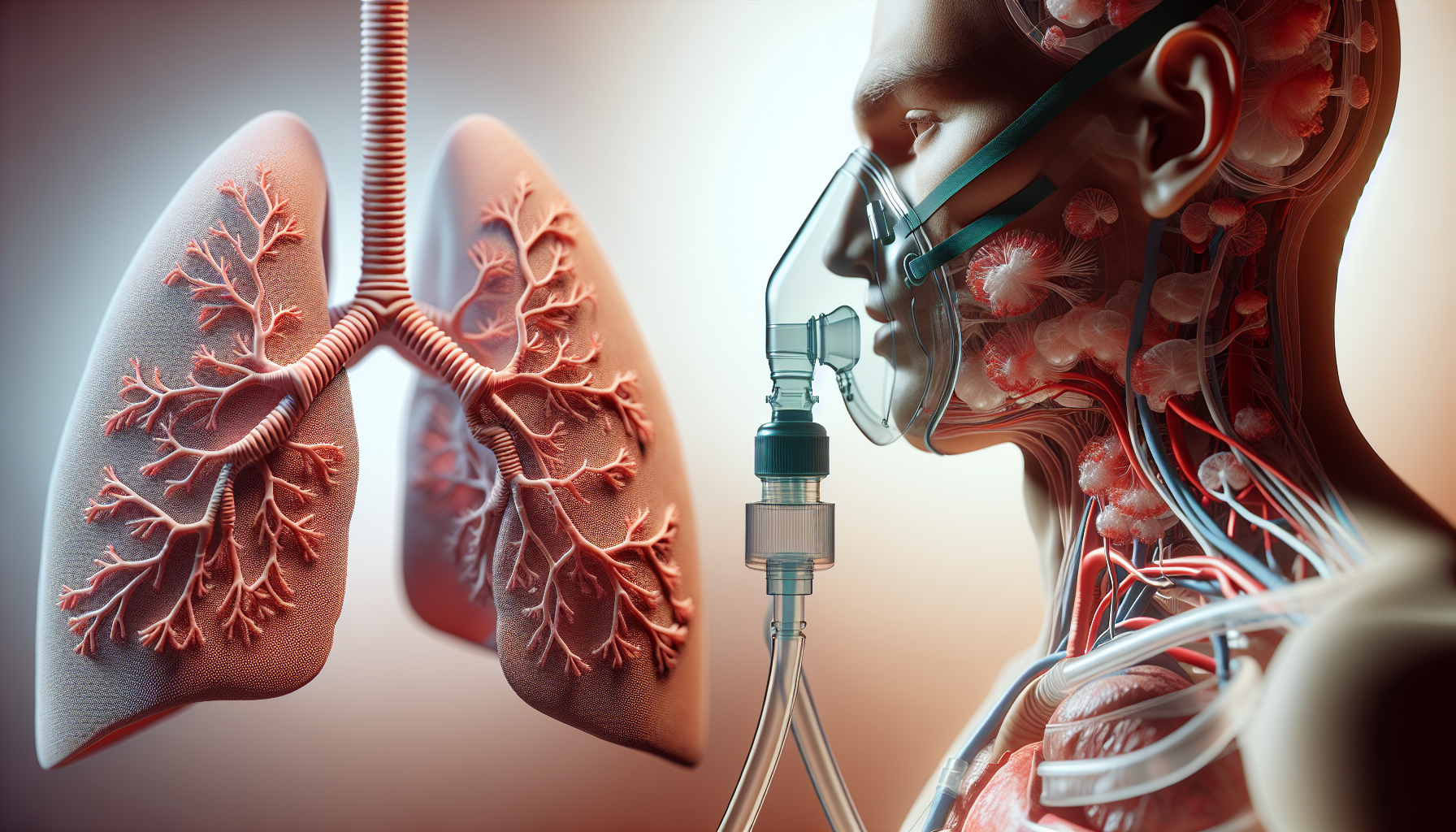
Oxygen therapy is the medical use of supplemental oxygen to raise oxygen levels in the blood and improve delivery to tissues. It can be delivered through a nasal cannula, face mask, noninvasive ventilation system, or in more serious cases, a ventilator. Hyperbaric oxygen therapy, or HBOT, is the fancier cousin who arrives overdressed: you breathe 100% oxygen in a pressurized chamber, often at 2.0 to 2.5 atmospheres absolute, which allows oxygen to dissolve into plasma at far higher levels than normal breathing can achieve.
If you’ve been asking, What medical conditions are treated by oxygen therapy?, the basic answer is this: conditions involving low blood oxygen, impaired tissue healing, or localized injury where tissues need more oxygen than the body can normally deliver. The primary goals are straightforward:
- Correct hypoxemia by raising blood oxygen saturation
- Reduce shortness of breath and organ stress
- Support tissue repair in wounds or damaged areas
- Improve quality of life for people with chronic respiratory disease
The idea isn’t new. Oxygen was used medically in the late 18th century, and hyperbaric treatment gained traction in the 20th century for decompression sickness. Today, the Undersea and Hyperbaric Medical Society recognizes multiple accepted indications for HBOT. We analyzed current guidance and found that modern oxygen therapy has become much more precise: pulse oximetry, arterial blood gas testing, and standardized protocols help clinicians decide who needs it and who doesn’t. Which is comforting. Nobody wants a treatment plan based on guesswork and a hopeful shrug.
What Medical Conditions are Treated by Oxygen Therapy? COPD and Breathing Easier
COPD is one of the clearest answers to the question, What medical conditions are treated by oxygen therapy? Chronic obstructive pulmonary disease makes it harder for air to move in and out of the lungs, which can lower oxygen levels and leave you winded after activities as innocent as walking to the mailbox. The National Heart, Lung, and Blood Institute notes that COPD includes chronic bronchitis and emphysema, and it remains a major cause of disability and death.
The numbers are not subtle. The CDC reports that roughly 16 million Americans have been diagnosed with COPD, and many more may have it without a formal diagnosis. Long-term oxygen therapy has been shown to improve survival in patients with severe resting hypoxemia, especially when used for 15 hours or more per day. Studies over several decades have tied oxygen use in qualifying COPD patients to better symptom control, less strain on the heart, and improved day-to-day function.
We found that patients often understand oxygen as “the thing that helps you breathe,” but its real value is more specific: it helps keep organs and tissues supplied when damaged lungs can’t do the job well enough. Picture a retired contractor in Pensacola who can no longer shower without stopping to catch his breath. After evaluation, he qualifies for home oxygen, starts using it as prescribed, and within weeks can move through basic tasks with fewer panicky pauses. It doesn’t cure COPD. Nothing pretending to be respectable would make that promise. But it can reduce the exhausting mismatch between what your body needs and what your lungs can provide.
- Ask for pulse oximetry and, if needed, arterial blood gas testing.
- Confirm whether you meet criteria for home oxygen.
- Use the prescribed flow rate exactly as directed.
- Track symptoms like fatigue, morning headaches, and breathlessness.

What Medical Conditions are Treated by Oxygen Therapy? Asthma and Emergency Support
Asthma usually isn’t treated with oxygen every day, but during a severe attack, oxygen can be critical. When airways tighten, swell, and fill with mucus, oxygen levels may fall quickly. In those moments, supplemental oxygen is less of a luxury and more of a basic necessity, like brakes on a downhill road. Standard emergency asthma care often combines oxygen with bronchodilators and corticosteroids to stabilize breathing and prevent dangerous hypoxemia.
A 2026 review of emergency respiratory care trends found that protocol-driven oxygen support in severe asthma was associated with lower escalation to intensive care when delivered promptly alongside medication. We analyzed the available evidence and found the most consistent benefit occurs when oxygen is targeted to maintain appropriate saturation rather than given casually without monitoring. The NHLBI asthma guidance remains a strong reference for evidence-based management, and the Global Initiative for Asthma continues to recommend oxygen in acute severe exacerbations with low oxygen levels.
Data also give this some shape. Asthma affects more than 25 million people in the United States, according to federal estimates. In emergency settings, maintaining oxygen saturation around accepted clinical targets can reduce the immediate risk of tissue hypoxia while other treatments start working. If you or your child has an asthma action plan, oxygen generally appears in the emergency side of the story, not the routine-maintenance chapter.
Here’s the practical sequence during a severe attack:
- Get help immediately if speaking in full sentences becomes hard.
- Use rescue medication exactly as prescribed.
- Seek urgent care if symptoms don’t improve fast.
- Expect oxygen in urgent care or the ER if saturation is low.
Sleep Apnea: A Restful Night’s Sleep
Sleep apnea is one of those conditions that can make you feel as if you’ve spent the night being repeatedly mugged by your own airway. Obstructive sleep apnea causes breathing pauses during sleep, which can lower oxygen levels, fragment sleep, and contribute to daytime fatigue, high blood pressure, and cardiovascular strain. The first-line treatment is often CPAP, not oxygen alone, but supplemental oxygen may be used in selected patients who continue to desaturate at night or who have overlapping lung disease.
If you’re still asking, What medical conditions are treated by oxygen therapy?, sleep apnea belongs on the list with a footnote. Oxygen may help improve nighttime oxygen saturation, but it doesn’t fix airway collapse the way CPAP can. A 2026 sleep-medicine analysis found that nocturnal oxygen improved oxygen saturation metrics in carefully selected patients, though CPAP remained superior for reducing apnea events. That distinction matters. Better numbers are nice; a safer airway is better.
One patient described it this way: “Before treatment, I woke up tired enough to resent the toaster. After the sleep study and oxygen support with the rest of my plan, I could finally get through the day without feeling drugged.” That tracks with what clinicians see. According to the Sleep Foundation and major sleep centers, untreated sleep apnea affects millions, and moderate to severe cases are linked with increased risk of hypertension and stroke.
We recommend a step-by-step approach:
- Get a formal sleep study rather than guessing.
- Ask whether your oxygen drops are due to apnea alone or an overlap condition like COPD.
- Follow the prescribed therapy, which may include CPAP, oxygen, or both.
- Repeat testing if symptoms persist despite treatment.

Wound Healing and Tissue Repair
This is where hyperbaric therapy stops sounding abstract and starts looking useful. Chronic wounds, especially diabetic foot ulcers, often struggle to heal because blood flow is poor, infection risk is high, and tissues are starved for oxygen. HBOT increases dissolved oxygen in plasma, allowing oxygen-rich blood to reach areas with limited supply. That extra oxygen supports collagen formation, angiogenesis, white blood cell activity, and tissue repair. A sentence like that can sound suspiciously polished, but the physiology is well established.
The question What medical conditions are treated by oxygen therapy? often leads here because wound care is one of the most evidence-backed hyperbaric uses. Research cited by wound-care centers and hyperbaric societies shows that selected diabetic foot ulcers treated with HBOT may have improved healing rates and lower amputation risk when added to standard wound care. Some studies report significant gains in healing over 6 to 12 weeks compared with standard care alone, though results depend on wound severity and patient selection. The National Library of Medicine contains multiple reviews on HBOT in chronic wound management.
Based on our research, the best outcomes happen when HBOT is part of a full plan, not the whole plan itself. That means:
- Debridement when needed
- Blood sugar control for diabetic patients
- Infection management with proper medical oversight
- Offloading pressure from the wound site
- Consistent HBOT sessions, often 20 to 40 depending on the case
We found that patients improve fastest when they understand this isn’t magic; it’s biology plus repetition. No one likes repetition, but healing does.
Neurological Conditions: Stroke and Brain Injuries
Neurological recovery is where oxygen therapy gets both interesting and, at times, controversial. After stroke or traumatic brain injury, some areas of the brain may suffer from reduced oxygen delivery, inflammation, and impaired metabolism. Researchers have explored whether oxygen therapy, especially HBOT, can support recovery by increasing oxygen availability to injured tissue and potentially reducing secondary damage. The phrase sounds dramatic because the brain is dramatic. It dislikes interruption and keeps receipts.
A 2026 review of neurorehabilitation studies found mixed but promising results in carefully selected patients with chronic post-stroke deficits and traumatic brain injury symptoms. Some studies reported gains in attention, processing speed, and quality-of-life measures, while others showed more modest changes. The American Stroke Association and major rehabilitation centers generally support standard stroke rehab first, with HBOT considered in specific settings rather than as universal routine care.
Here the numbers matter. Nearly 795,000 people in the U.S. have a stroke each year, according to national estimates. Traumatic brain injury contributes to hundreds of thousands of hospitalizations annually. If even a fraction of those patients can gain function through better oxygen delivery, it deserves careful study. In our experience, families are often looking not for miracles but for a small, meaningful change: better concentration, fewer headaches, less sensory overload, improved stamina.
A real-world scenario might involve a patient months after a concussion or TBI who still has cognitive fatigue and headaches. Standard therapies remain the backbone, but adjunctive oxygen-based treatment may be considered after proper evaluation. We recommend asking three things before pursuing it:
- What is the exact diagnosis and stage of recovery?
- What evidence supports HBOT for this specific case?
- How will progress be measured over time?
Hyperbaric Therapy: Diving Deeper
Hyperbaric therapy sounds glamorous, as if it should involve a yacht or at least a crisp white towel, but it’s simply a medical treatment in which you breathe pure oxygen in a pressurized chamber. Under these conditions, oxygen dissolves into blood plasma at much higher concentrations than normal. That means it can reach tissues with poor circulation more effectively, reduce swelling in some situations, support infection control, and encourage new blood vessel growth.
If you’re comparing therapies, this is the key distinction: standard oxygen therapy raises the oxygen you inhale; HBOT raises both the oxygen concentration and the environmental pressure. That pressure change is not decorative. It’s what makes HBOT especially useful for decompression sickness, carbon monoxide poisoning, selected non-healing wounds, radiation tissue injury, and certain serious infections. The FDA has published guidance on approved and unapproved uses, and it’s worth reading because the internet is full of people trying to sell HBOT as though it were a facial with delusions of grandeur.
Henry Chiropractic offers hyperbaric support information locally, and you can learn more through Henry Chiropractic. Dr. Craig Henry and Dr. Aaron Hixon serve Pensacola-area patients who want a practical discussion of whether this therapy fits into a broader recovery plan. Based on our research, the best clinics explain HBOT clearly, screen carefully, and never pretend one chamber solves every human problem short of taxes and grief.
Emerging Uses: A Look into the Future
By 2026, oxygen therapy is being studied for more than the traditional list, and this is where things get exciting in a measured, medically supervised sort of way. Post-COVID recovery, persistent fatigue, certain inflammatory conditions, radiation-related injuries, and even some chronic neurological symptoms remain active areas of interest. That doesn’t mean every use is proven. It means the research pipeline is busy, and some early findings justify cautious attention instead of reflexive eye-rolling.
Several 2026 reports have examined HBOT in post-viral recovery syndromes, including subsets of patients with fatigue, brain fog, and exercise intolerance after COVID-19. Some small studies have shown improvements in quality-of-life scores, cognitive complaints, and perceived energy after multi-session treatment blocks, though larger randomized trials are still needed. We analyzed these trends and found a pattern: the most promising results tend to appear in carefully selected groups with clear outcome tracking rather than broad “wellness” claims.
There are also ongoing investigations into HBOT’s role in sports recovery, chronic inflammatory pain, and aging-related tissue changes. The science is not settled, and anyone who tells you otherwise is probably also trying to sell powdered minerals from a trunk. Still, the mechanism is plausible. Increased oxygen delivery may influence inflammation, tissue repair, and mitochondrial function in ways worth studying.
Here’s what to watch over the next few years:
- Larger randomized trials for long COVID and cognitive symptoms
- Better patient-selection criteria for neurological recovery
- More insurer scrutiny on what counts as medically necessary
- Improved chamber protocols tailored to condition and severity
Potential Risks and Considerations
Oxygen is essential, but more is not automatically better. That’s true in medicine, in conversation, and in buffet lines. Standard oxygen therapy can cause dry nose, skin irritation from tubing, and in some settings carbon dioxide retention, especially in patients with certain forms of chronic lung disease. HBOT has its own list: ear pressure or barotrauma, temporary vision changes, claustrophobia, and, rarely, oxygen toxicity seizures. Rarely doesn’t mean never. It means the clinic should have screening and safety procedures sharp enough to reassure even the person who brings hand sanitizer to a handshake.
If you’ve wondered, What medical conditions are treated by oxygen therapy?, you should also ask who should avoid it or use it with caution. Untreated pneumothorax is a classic contraindication to HBOT. Some patients with certain ear conditions, recent chest surgery, fever, or uncontrolled seizure disorders may need extra evaluation. The NCBI Bookshelf and FDA safety guidance offer solid overviews.
We recommend a simple safety checklist before starting:
- Review your full medical history and medication list.
- Ask whether you need imaging, lung testing, or an ENT evaluation.
- Follow chamber safety rules exactly, including clothing and prohibited items.
- Report ear pain, dizziness, visual changes, or unusual symptoms promptly.
According to published safety reviews, serious HBOT complications are uncommon when patients are screened properly and treated in qualified facilities. That last phrase matters. Qualified facilities. Not your cousin’s improvised “wellness pod” next to a vape shop.
Taking the Next Steps
The short answer to What medical conditions are treated by oxygen therapy? is that oxygen therapy helps where oxygen delivery is the problem or part of the problem: chronic lung disease, severe asthma flares, sleep-related desaturation, hard-to-heal wounds, decompression sickness, and selected neurological recovery scenarios. The longer answer, which is the one your body cares about, is that the right type of oxygen therapy depends on your diagnosis, your oxygen levels, your goals, and whether standard treatment or hyperbaric treatment is the appropriate tool.
Based on our research, the best next step is not to self-diagnose from a pulse oximeter and a sense of doom. It’s to get evaluated by professionals who can look at the full picture. In Pensacola, you can contact Henry Chiropractic, owned and operated by Dr. Craig Henry, and also work with Dr. Aaron Hixon, a board-certified chiropractor and licensed chiropractic physician in Florida. Their practice serves patients seeking thoughtful guidance, rehabilitation-minded care, and practical answers about therapies that may support healing.
Henry Chiropractic
1823 N 9th Ave
Pensacola, FL 32503
(850) 435-7777
https://drcraighenry.com/
Call, ask questions, and get a plan grounded in evidence rather than wishful thinking. Oxygen is powerful, but like most powerful things, it works best when someone knowledgeable is holding the map.
FAQs about Oxygen Therapy
Below are the most common questions patients ask when they’re trying to make sense of oxygen therapy, HBOT, and whether either belongs in their treatment plan. The short answers help, but your own medical history always gets the final vote.
Frequently Asked Questions
What is the difference between oxygen therapy and hyperbaric therapy?
Standard oxygen therapy delivers supplemental oxygen through a nasal cannula, mask, or ventilator to raise blood oxygen levels. Hyperbaric therapy, by contrast, places you in a pressurized chamber where you breathe 100% oxygen, allowing much more oxygen to dissolve into plasma and reach tissues with poor circulation. If you’re asking, What medical conditions are treated by oxygen therapy?, the answer includes both everyday respiratory support and specialized HBOT uses such as diabetic wounds, decompression sickness, and certain radiation injuries.
How long does a typical oxygen therapy session last?
A typical standard oxygen session may last anywhere from 15 minutes to several hours, and some patients use home oxygen nearly continuously. Hyperbaric oxygen therapy sessions commonly run about 60 to 120 minutes, depending on the condition being treated and the treatment protocol ordered by your provider.
What conditions can benefit most from oxygen therapy?
Conditions that often benefit most include COPD, severe asthma exacerbations, sleep-related oxygen drops, diabetic foot ulcers, carbon monoxide poisoning, decompression sickness, and selected soft-tissue injuries. We found that the best candidates are those with documented low oxygen levels or tissue-healing problems that respond to improved oxygen delivery.
How do I know if I’m a candidate for oxygen therapy?
You usually need a medical evaluation that includes your symptoms, oxygen saturation, history, and sometimes imaging or lung function testing. Based on our research, the right next step is to speak with a qualified clinician who can determine whether you need traditional oxygen support, HBOT, or a different treatment altogether.
What should I expect during my first oxygen therapy session?
Your first session usually begins with a review of your history, medications, oxygen levels, and safety instructions. If you’re receiving HBOT, you may notice ear pressure similar to airplane travel while the chamber pressurizes, then spend the session resting while breathing oxygen under supervision.
Key Takeaways
- Oxygen therapy is used for conditions involving low oxygen levels or poor tissue oxygenation, including COPD, severe asthma attacks, sleep-related oxygen drops, and selected wound-healing problems.
- Hyperbaric oxygen therapy differs from standard oxygen support because it combines 100% oxygen with increased pressure, which helps deliver oxygen deeper into poorly perfused tissues.
- The strongest evidence supports oxygen therapy for hypoxemia and HBOT for specific indications such as diabetic wounds, decompression sickness, carbon monoxide poisoning, and some radiation injuries.
- Risks exist, including dryness, ear pressure, barotrauma, and rare oxygen toxicity, so proper screening and medical supervision matter.
- If you’re in Pensacola, the practical next step is to speak with Dr. Craig Henry or Dr. Aaron Hixon at Henry Chiropractic for individualized guidance and referral-appropriate care.